Imagine being a parent and watching your child hear the sound of your voice for the very first time — not as an infant, but at age four or six or ten. That moment, until recently, was made possible only by cochlear implants: surgically placed electronic devices that bypass the damaged ear entirely. But on April 23, 2026, the FDA approved a fundamentally different approach. Instead of routing around the problem, it fixes it — at the level of the gene.
The drug is called Otarmeni (lunsotogene parvec-cwha), and it is the first gene therapy ever approved for genetic hearing loss. Developed by Regeneron Pharmaceuticals (which acquired Decibel Therapeutics, the therapy's original developer), Otarmeni targets a very specific and well-understood cause of congenital deafness: a broken copy of the OTOF gene. The results from clinical trials are striking. In some treated children, hearing went from profound deafness to the ability to hear a whisper.
This is how it works — and why it matters.
What Is OTOF-Related Deafness?
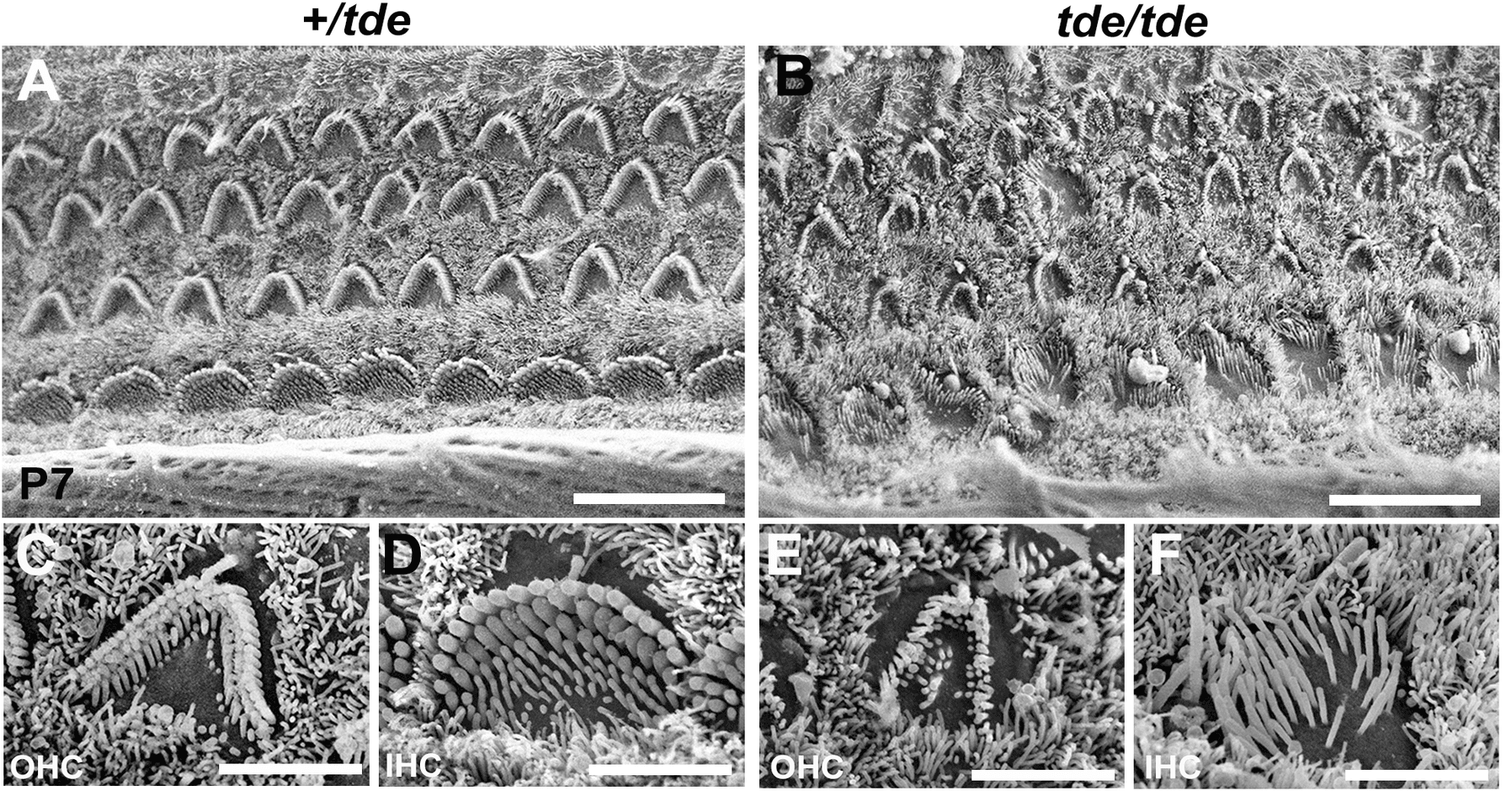
Inside the inner ear, nestled in a fluid-filled spiral structure called the cochlea, are roughly 3,500 cells called inner hair cells. Despite the name, these are not hairs at all — they are exquisitely sensitive sensory neurons that convert sound vibrations into electrical signals the brain can interpret. They are, in effect, the microphones of the auditory system.
But a microphone is useless without a cable connecting it to a speaker. That cable, in the inner ear, is a protein called otoferlin.
When a sound wave causes an inner hair cell to vibrate, otoferlin acts as a molecular trigger: it senses the surge of calcium ions that follows mechanical stimulation and responds by fusing tiny glutamate-filled vesicles with the cell's outer membrane. This releases the neurotransmitter glutamate into the synapse, which activates the auditory nerve, which carries the signal to the brain. Remove otoferlin, and the hair cells remain physically intact — but they go silent. The microphone exists; the cable is missing.
Otoferlin is encoded by the OTOF gene. When a child inherits two nonfunctional copies of this gene — one from each parent, a pattern called biallelic variants — they produce no functional otoferlin and are born with severe-to-profound sensorineural hearing loss. This condition, sometimes called DFNB9, is one of the most common forms of congenital genetic deafness and accounts for an estimated 2–8% of all congenital hearing loss worldwide.
In the United States, approximately 50 infants are born each year with OTOF mutations. Globally, the number of people living with this specific form of congenital deafness is estimated at around 200,000.
One important distinction: this is not the kind of hearing loss caused by loud noise, aging, or infection. OTOF-related deafness is a genetic condition present from birth, caused by a single identifiable molecular defect. That precision is exactly what makes it a tractable target for gene therapy.
How Does Gene Therapy Restore Hearing?
The core idea is straightforward: deliver a working copy of the OTOF gene directly into the inner hair cells where it is needed.
The delivery vehicle is an adeno-associated virus (AAV) vector. Think of an AAV as a microscopic delivery truck. Scientists take the shell of this naturally occurring, non-disease-causing virus, strip out its own genetic cargo, and load it with the therapeutic gene instead. The virus's protein coat — its capsid — acts like an address label, guiding it to specific cell types. Once inside the target cell, the genetic payload is released and the cell begins producing the protein it was previously missing.
There is one significant technical challenge with the OTOF gene: it is large. The coding sequence of the OTOF gene is roughly 6,000 base pairs — too big to fit inside a single AAV vector, which has a strict packaging limit of about 4,700 nucleotides. Standard AAV-based gene therapies sidestep this problem by targeting smaller genes. For otoferlin, researchers at Decibel Therapeutics (now part of Regeneron) needed a more creative solution.
Their answer was the dual-AAV vector system. Rather than cramming the entire gene into one vehicle, they split the OTOF coding sequence across two separate AAV vectors. When both vectors enter the same cell — which they do with high efficiency when injected at sufficient concentration — the two halves of the gene recombine inside the nucleus through a process called concatemerization, and a complete, functional copy of the otoferlin protein is produced. It is, in molecular terms, a two-truck delivery: each truck carries half the cargo, and the cargo only works when both halves arrive at the same destination.
Otarmeni holds a significant regulatory distinction: it is the first dual-AAV gene therapy ever approved by the FDA.
Administration is a single-dose procedure: Otarmeni is infused directly into the cochlea (intracochlear injection) under general anesthesia, using a surgical approach similar to the one used for cochlear implantation. The surgery can be performed in one ear or both, and can be done even in very young infants. Critically, the AAV vector used in Otarmeni is engineered with a cell-specific promoter — a genetic switch that restricts otoferlin production almost exclusively to inner hair cells, the cells that actually need it. This cell-targeting precision limits off-target activity elsewhere in the body.
What Did the Trial Show?
The pivotal clinical trial behind Otarmeni is called the CHORD trial (NCT05788536) — an open-label, multicenter, Phase 1/2 study conducted across multiple sites. It enrolled 20 children and infants ranging from 10 months to 16 years of age, all with confirmed biallelic OTOF mutations and severe-to-profound sensorineural hearing loss.
The results were remarkable.
80% of participants (16 of 20) improved their hearing enough to meet or surpass the trial's primary endpoint — defined as achieving a pure tone audiometry (PTA) threshold of 70 decibels hearing level (dB HL) or better at 24 weeks after treatment. One additional participant reached this threshold by week 48, raising the responder rate further. In practical terms, 70 dB HL represents the ability to perceive conversational speech at close range — a significant functional gain for children who previously could not hear anything below 90 dB HL.
Among the 12 participants followed out to 48 weeks, 42% achieved normal hearing — defined as a threshold of 25 dB HL or better, which is the level at which a person can hear a soft whisper from a few feet away. All participants who responded at 24 weeks maintained their response at 48 weeks, suggesting the improvement is durable rather than transient.
70% of participants also demonstrated an auditory brainstem response (ABR) at or below 90 dB by week 24, confirming that the sound signal was traveling along the auditory nerve to the brain — not just being detected at the ear.
The therapy was well tolerated. No adverse events or serious adverse events were attributed to Otarmeni itself. The surgical procedure was consistent with cochlear implantation surgery, a routine procedure in pediatric ear-nose-throat practice.
It is important to be honest about what the trial did not show: with only 20 participants, the study is small by the standards of most drug approvals. Otarmeni received accelerated approval from the FDA, meaning it was approved based on these early results, with a commitment to verify the clinical benefit in a larger confirmatory portion of the CHORD trial. Continued approval is contingent on that confirmatory data. That is not a weakness unique to Otarmeni — it is the standard regulatory pathway for rare disease therapies, where assembling large trial cohorts is practically impossible when only 50 babies per year are born with the condition in the entire country.
Why This Matters Beyond One Drug
The approval of Otarmeni is significant for reasons that extend well beyond OTOF-related deafness.
First, it establishes the dual-AAV platform as a viable, approvable gene therapy approach. Until now, the large-gene problem was a hard ceiling on what AAV-based gene therapy could treat. By demonstrating that dual-AAV works safely and effectively in humans — and by earning FDA approval — this therapy clears a technical path for gene therapies targeting dozens of other large-gene disorders: GJB2-related deafness, Usher syndrome, and beyond.
Second, the CHORD trial extended the known treatment window for this type of gene therapy. Participants as old as 16 received clinical benefit, demonstrating that the inner hair cells, even in older children, retain enough biological capacity to respond when otoferlin is supplied. Earlier animal studies had suggested a narrow developmental window; the human data suggests that window may be wider than feared.
Third, Otarmeni is being made available at no cost to clinically eligible patients in the U.S. — an unusual and notable access decision by Regeneron, particularly in an era when gene therapies routinely carry price tags of $1 million or more. The drug was also approved under the FDA Commissioner's National Priority Voucher (CNPV) pilot program, which enables accelerated review for therapies addressing serious rare conditions. Otarmeni is the sixth product approved under this program and the first gene therapy to receive approval through it.
It is also worth naming what Otarmeni does not do. It will not help the millions of people with age-related hearing loss, noise-induced hearing loss, or deafness caused by mutations in any gene other than OTOF. The population it addresses is small and biologically specific. Genetic testing is required to confirm eligibility. And like all gene therapies, its long-term durability — beyond the roughly one-year data available now — remains to be demonstrated.
The Bottom Line
The FDA's April 2026 approval of Otarmeni marks a genuine milestone: the first gene therapy to restore hearing in humans, built on a novel dual-AAV platform that solved a long-standing technical barrier in the field. For children born deaf because of a broken OTOF gene, it offers something that no drug has ever offered before — not amplification, not workarounds, but a functional repair of the underlying molecular defect. Eighty percent improved significantly; nearly half now hear whispers. The technology that made this possible will almost certainly be used to address other forms of genetic hearing loss — and other large-gene diseases — in the years ahead.
Sources: FDA press announcement · Regeneron investor release · The Hearing Review · NEJM — DB-OTO trial results · CGTlive — accelerated approval